Hands on Learning
During the second week of my internship, I was able to move beyond observation and begin actively connecting what I see in the clinic to what I am learning in the classroom at Cornell. Each day offered new insight into how physical and occupational therapists assess, treat, and build trust with their patients. I asked a lot of questions on how they come up with the exercises, how they adjust them for at home exercises and to feel it more on the targeted muscle. I took note on how they spoke to their patients from the first time meeting them to a few sessions in. It’s important to have a good relationship with the patients. On Day 6, one of the physical therapists spent time teaching me different ways to stretch the neck muscles while explaining the function of each muscle group. I am also learning specific clinical skills such as joint mobilizations, weight-bearing exercises, and proper crutch walking. In addition, I have been introduced to the technology therapists use to create recovery programs and stay up to date with current physical therapy guidelines and research. I learned how to feel for muscle knots and what techniques can be used to help release them, with a strong focus on the upper back and trapezius muscles. This experience directly connected to my anatomy class, as I was able to visualize muscle structures.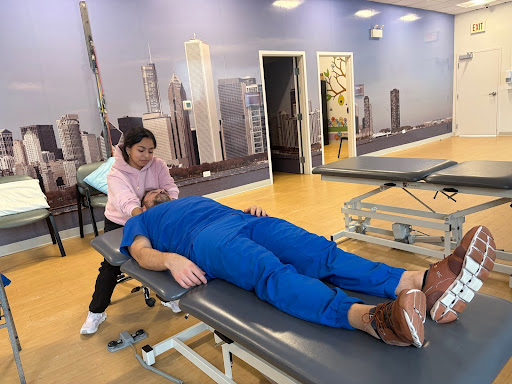
In this image, I am stretching the deeper neck muscles. The physical therapist palpated on me prior to teach me where I should feel the stretch and where to place my hands.
Throughout the week, I was exposed to a wide range of patient evaluations, including hip, shoulder, knee, and ankle assessments. I paid close attention to how physical therapists test range of motion and how they communicate throughout the evaluation process. The PT explained to me how important it is to build trust so that the patient can feel more comfortable. This then led me to ask questions about how therapists build relationships with patients and establish trust. I learned that communication, empathy, and consistency are just as important as technical skill in patient care. This reinforced the importance of patient-centered physical therapy and showed me that successful treatment depends on understanding both physical limitations and emotional needs.
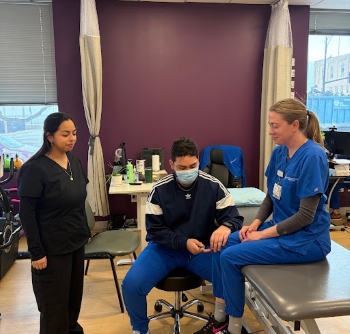
This image shows a Physical Therapist and Speech Pathologist. The PT was showing me different ways to test for reflexes.
My coursework at Cornell has strongly supported my ability to understand and engage with what I am seeing in the clinic. Classes such as anatomy and child development directly connect to my daily experiences. For example, learning about muscle groups and their functions in anatomy has helped me better understand neck and upper back treatments, while child development coursework has helped me recognize developmental stages when observing occupational therapy sessions with children. Cornell has also prepared me to ask thoughtful questions, communicate professionally, and reflect critically on my experiences. Rather than simply observing, I am able to actively connect theory to practice, which has made this internship more meaningful and educational. Personally, this experience has helped me gain confidence in clinical environments and has allowed me to see myself in a future healthcare role. It has also helped clarify the type of work environment I would like after college.
Through this internship, I am learning about the culture of the rehabilitation field and the importance of teamwork in patient care. The clinic environment emphasizes collaboration, patient-centered care, and continuous learning. Therapists support one another, share knowledge, and adapt treatments to meet patient goals, which has created a positive and motivating work atmosphere. Understanding the history and evolution of physical and occupational therapy has also shown me how research, technology, and patient advocacy continue to shape the field.